Download The Ultimate Guide to Sustainable Dentistry eBook
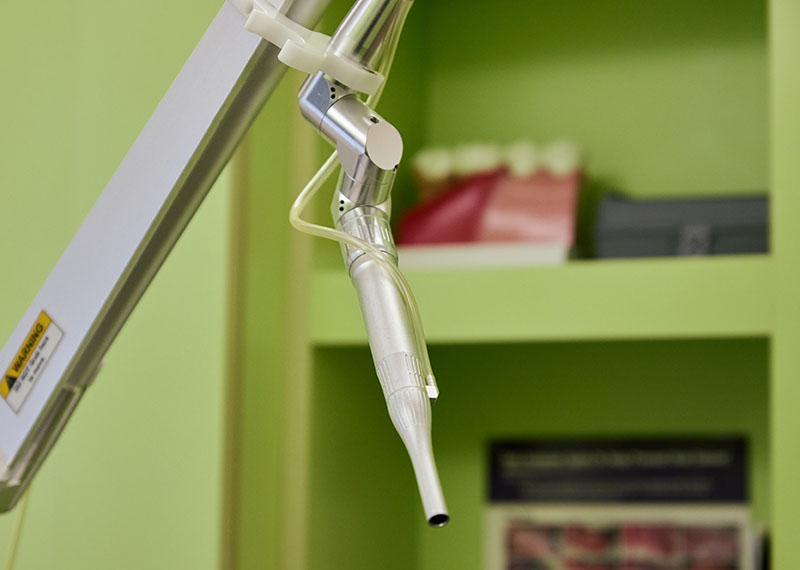
A CO² laser uses carbon dioxide to generate energy and its wavelength. It uses this energy to vaporize the water found in soft tissues, providing quick, accurate cutting—and bleeding stops in an instant. Lasers are widely used medicine—and for good reason. They are well-suited for dental procedures including frenectomies, gingivectomies, excisions, and soft tissue procedures around dental implants. The MicroSpeed technology makes lasers such as this one as one of the gentlest, and most highly effective, tools at our disposal.
How Do CO2 Lasers Work?
Dentists have used CO² lasers for more than 25 years, but they have been available in medicine since the early 1970s. These devices are flexible, versatile, and give the operator much more control, emitting a 10,600 nm infrared wavelength—which water easily absorbs. These types of lasers are currently for soft tissue uses only, and are continuous wave lasers that can be operated in gated wave modes—including what are termed “superpulsed” modes. The CO² gas is stored in a chamber with nitrogen and an electric current pumps helium with the active medium.
What Are CO2 Lasers Used to Treat?
Because they are efficient and keep bleeding halted, CO² lasers are excellent tools for incising tissue for multiple purposes. This includes incisional and excisional biopsies, frenectomy, gingivectomy, pre prosthetic procedures—all made more difficult when bleeding gets in the way. For these processes, sutures are rarely needed; the controlled thermal effects and sealing of nerve endings often makes for a very comfortable post-operative experience for the patient.
Most recently, variations of the CO² laser with hard tissue capabilities have become available for use. This laser’s CO² molecule uses an oxygen isotope that creates a beam at 9300 nm. This means it has a high absorption affinity for hydroxyapatite—allowing for teeth to be vaporized. Because hard tissue ablation with the 9300 nm CO² laser is a photothermal event, and not photoacoustic, it generates much higher temperatures and much higher pulse rates are needed to cut.
 Request Appointment
Request Appointment